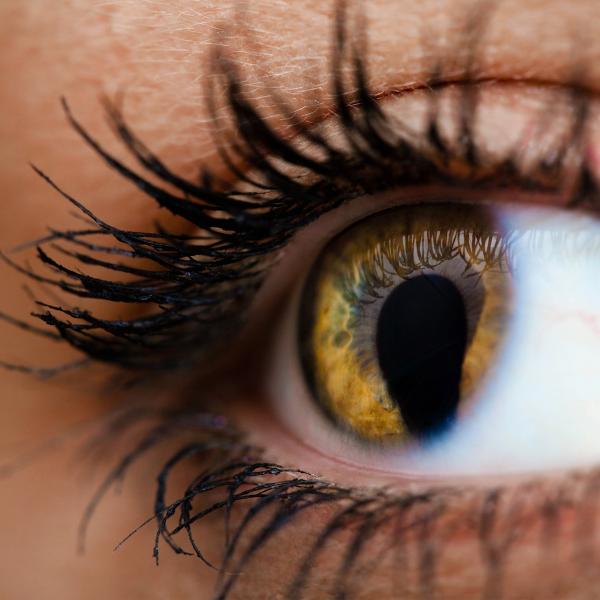
What is coloboma?
Coloboma is an eye condition that people are born with. It happens when part of the tissue that makes up the eye is missing. It can affect 1 or both eyes.
If your child has coloboma, talk to your doctor about the best plan for their care. There are treatments that can help them make the most of their vision.
What are the types of coloboma?
Different types of coloboma can affect different parts of the eye, including the:
- Iris (colored part of the eye)
- Uvea (layer of the eye that contains the iris)
- Lens (clear inner part of the eye that helps the eye focus)
- Retina (light-sensitive tissue lining the back of the eye)
- Macula (part of the retina needed for central vision
- Optic nerve (nerve that connects the eye to the brain)
Coloboma can also affect the eyelids.
What are the symptoms of coloboma?
Some people with coloboma have no symptoms. Others may have problems with their vision, including:
- Vision loss or blindness
- Low vision
- Sensitivity to light
Some colobomas are visible. For example, iris coloboma can make the pupil (the round opening at the center of the iris) look more like a keyhole or teardrop.
What causes coloboma?
Coloboma happens when a baby’s eye doesn’t develop normally during pregnancy because of abnormal or changed genes that affect eye development. Coloboma sometimes runs in families. Environmental factors, such as drinking alcohol during pregnancy, may also increase a baby’s risk for coloboma.
Coloboma often happens together with conditions that affect other parts of the body, like CHARGE syndrome and Wolf-Hirschhorn syndrome.
How will my child’s doctor check for coloboma?
Coloboma may be visible when your baby is born, so the doctor may be able to diagnose it by looking at their eyes during an exam. If your child’s coloboma isn’t visible, the doctor can diagnose it by doing a comprehensive dilated eye exam.
What’s the treatment for coloboma?
Treatment can’t replace the part of the eye that’s missing because of coloboma. But there are treatments that can help people with coloboma make the most of their vision.
-

Glasses or contacts. People with coloboma who have refractive errors may need to wear eyeglasses or contact lenses to see more clearly. People with iris colobomas can also wear colored contact lenses to make their pupils look rounder.
-

Surgery. People with iris colobomas sometimes get surgery to make their pupils look rounder. If you’re concerned about the appearance of your eyes, ask your eye doctor about your options.
-

Low vision aids. If your coloboma causes vision loss that can’t be corrected with glasses or contacts, you can use special devices to help you see better. A low vision specialist can help you identify the right devices for you and teach you how to use them.
-

Eye patch or eye drops. Children who have coloboma in only 1 eye may need to wear an eye patch or use special eye drops to prevent amblyopia (lazy eye).
Children and adults may need treatment for other eye conditions related to coloboma, such as cataracts or glaucoma.
If your child has coloboma, it’s important to talk to their doctors about the best plan for their care. Children with coloboma often need specialized care and therapy to help them grow and develop.
Other eye conditions related to coloboma
People with coloboma may also have problems like:
- Microphthalmia (unusually small eyes)
- Cataract (a cloudy area in the lens of the eye)
- Glaucoma (a group of eye diseases that can cause vision loss or blindness)
- Refractive errors (like nearsightedness or farsightedness)
What's the latest research on coloboma?
NEI researchers are studying the genes related to the type of coloboma that affects the uvea to learn more about what causes it.