
Emily Chew, M.D., with clinical trials participant.
The development of new therapies and cures would be impossible without patients volunteering for clinical research studies. In exchange, volunteers often receive care based on the latest research, while gaining the satisfaction of helping others. That was the case with David, a research nurse who has had type 1 diabetes since he was 11 years old. (He asked that we not use his full name.) Now 66, he owes his 20/20 vision to his participation in clinical research funded by the National Eye Institute (NEI), a part of the National Institutes of Health.
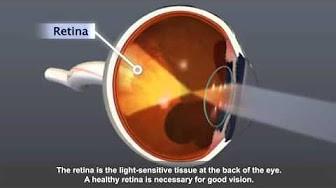
Since he was in his 20s, David has been treated for diabetic retinopathy, the leading cause of blindness in U.S. adults. This complication of diabetes damages tiny blood vessels in the light-sensing tissue in the back of the eye called the retina. Progression to more advanced proliferative diabetic retinopathy causes the growth of fragile blood vessels that can affect vision when they bleed into the eye. These abnormal blood vessels can also leak fluid and swell the central part of the retina, a condition called macular edema that can occur at any stage of diabetic retinopathy.

David undergoes examination of his retina.
“Without treatment, people with proliferative diabetic retinopathy have about a 50-percent chance of going blind in five years,” said Emily Y. Chew, M.D., NEI deputy clinical director at the NEI Eye Clinic within the NIH Clinical Research Center in Bethesda, Maryland. Chew was an investigator in the landmark NEI-funded Early Treatment of Diabetic Retinopathy Study (ETDRS), which ran from 1979-1985. The study found that laser treatment of abnormal retinal blood vessels may reduce rates of severe vision loss from diabetic retinopathy by up to 95 percent.
Laser surgery stops blood vessels from leaking or swelling by cauterizing tiny areas of the retina.
David participated in the ETDRS and the ETDRS follow-up. “We’re very fortunate to have people like David be part of this research,” said Chew, who has been actively involved in David’s treatment for more than a decade. She explained that participants are essential to help move research forward, and there’s an important dialogue throughout the process. “We get his input on everything about his care.”

Chew shows David an image of his retina.
Over the years as a clinical trials participant, David has witnessed the evolution of laser therapy. In fact, he was the first patient at NEI treated with a new device that delivers multiple laser burns at a time. “It’s much quicker,” noted David.

David’s retina. Grey spots are from laser treatments.
David also has been treated with anti-VEGF, a drug that prevents or slows the growth of abnormal retinal blood vessels. In 2010, the NEI-funded Diabetic Retinopathy Clinical Research (DRCR) Network showed that eye injections of the anti-VEGF drug Lucentis (ranibizumab) is effective for diabetic macular edema. The DRCR later compared the most commonly used anti-VEGF drugs—Lucentis, Avastin (bevacizumab), and Eylea (aflibercept)—for diabetic macular edema and found that all three substantially improve vision. Eylea outperformed the others when vision loss was moderate or worse. Proliferative diabetic retinopathy can also be effectively treated with anti-VEGF, the DRCR Network found in 2016. David received an anti-VEGF injection for a vitreous hemorrhage—bleeding into the gel-like center of the eye called the vitreous. When he saw salt-and-pepper spots floating in his vision, he promptly sought treatment at the NEI Eye Clinic.
Participation in clinical research has given David access to state-of-the-art treatment, but it has also helped him stay focused on the most effective way to prevent diabetes-related vision loss: managing diabetes.
“The key to beating diabetic retinopathy is good glucose control,” emphasized Dr. Chew. “There’s nothing like it. Maintaining good blood sugar levels can result in a 50-percent reduction in the progression of retinopathy. Managing blood pressure is also important.
One part of David’s routine is bike riding. “My wife and I try to ride every weekend,” he explained. And not just for short rides. “We’ve done a couple longer races, even one 100 miles.” He added, it’s not easy to keep up the exercise and diet, but everyone with diabetes must manage their disease.
NEI’s National Eye Health Education Program recommends these important steps to help people with diabetes keep their health on TRACK:
- Take your medications as prescribed by your doctor.
- Reach and maintain a healthy weight.
- Add physical activity to your daily routine.
- Control your ABC’s—A1C, blood pressure, and cholesterol levels.
- Kick the smoking habit.
For more details on diabetic retinopathy and other diabetic eye diseases, visit https://nei.nih.gov/health/diabetic/retinopathy.
Monitoring and early detection are key to preventing vision loss from diabetic retinopathy. There are no symptoms in early stages of the disease. Current guidelines suggest that people with type 1 diabetes have annual screenings for diabetic retinopathy starting five years after disease onset. Those with type 2 diabetes should have a comprehensive dilated eye exam at the time of diagnosis and annually after that.
“The challenge for us as clinicians has always been to provide adequate screening for retinopathy before visual symptoms appear,” explained Henry E. Wiley, M.D., a staff clinician who is leading the DRCR site at the NEI Eye Clinic. People with diabetes are also at greater risk of cataract and glaucoma.
The burden of diabetes and related eye diseases is heavy. An estimated 30.3 million people in the U.S have diabetes. Average medical expenditures for people with diabetes is about $13,700 per year, with about $7,900 attributable to diabetes.1
Originally funded by the NEI and the National Institute on Diabetes and Digestive and Kidney Diseases (NIDDK), the DRCR Network continues its clinical research into diabetic retinopathy. The Network formed in 2002 and partners with more than 350 physicians practicing at more than 140 clinical sites across the country. About 10,000 patient volunteers have participated in DRCR Network studies, according to Adam R. Glassman, M.S., principal investigator of the DRCR Network Coordinating Center at the Jaeb Center for Health Research.
“We’re now launching a study that will help us determine if we can treat diabetic retinopathy with anti-VEGF drugs at earlier stages of the disease,” said Wiley. The clinical trial is underway at DRCR sites.
David may be ineligible for this trial, but he’s grateful for the great care he’s received through his participation in clinical research. “I participated in every research study I could get my hands on,” he said. And because that care was part of research studies, it was all free.
For more information on how to join a study, visit https://nei.nih.gov/eyeclinic/join. To learn more about diabetic eye diseases, join the NEI and NIDDK for a Twitter chat on Thursday, November 16, 1:00-2:00 p.m. Eastern Time.
Reference:
Economic costs of diabetes in the U.S. in 2012. Diabetes Care 36, 1033-1046, doi:10.2337/dc12-2625 (2013). Pubmed
###
NEI leads the federal government’s research on the visual system and eye diseases. NEI supports basic and clinical science programs to develop sight-saving treatments and address special needs of people with vision loss. For more information, visit https://www.nei.nih.gov.
About the National Institutes of Health (NIH): NIH, the nation’s medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit http://www.nih.gov/.
NIH…Turning Discovery Into Health®

@NatEyeInstitute and @NIDDKgov will host a Twitter chat on diabetic eye disease.